
Lower Back Pain Treatment: What Actually Works
Lower back pain treatment is something nearly every adult will need at some point — around 8 out of 10 people experience it in their lifetime. For 16 million Americans, it becomes a chronic, ongoing struggle.
Here’s a quick overview of the most effective treatment options:
| Treatment Type | Best For | Timeline |
|---|---|---|
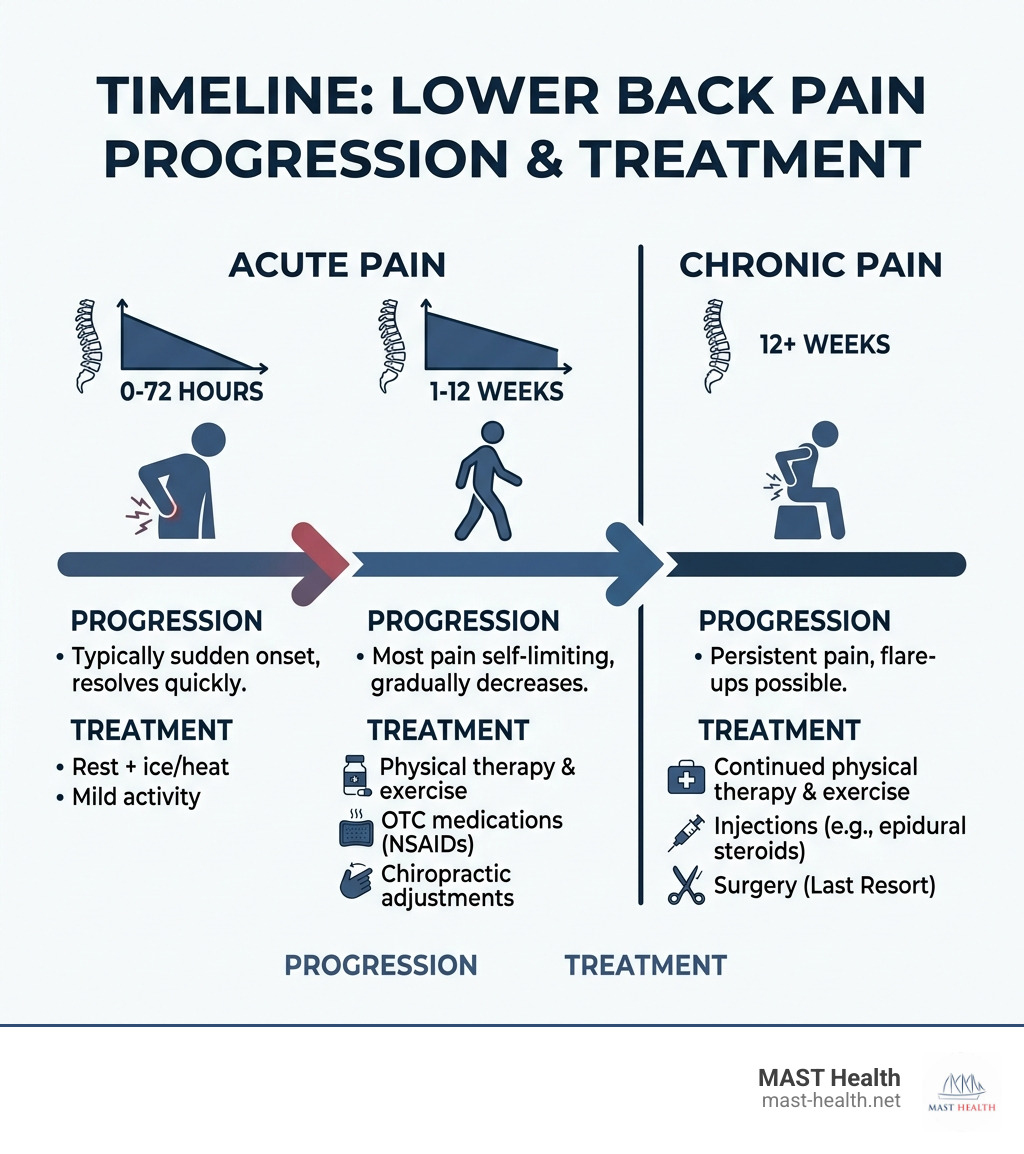
| Rest + ice/heat | Acute pain (first 72 hours) | Days |
| OTC medications (NSAIDs) | Mild to moderate pain | Days to weeks |
| Physical therapy & exercise | Acute and chronic pain | Weeks to months |
| Chiropractic adjustments | Spinal alignment, nerve compression | Weeks |
| Injections (e.g., epidural steroids) | Nerve-related or persistent pain | Short-term relief |
| Surgery | Structural issues after all else fails | Last resort |
The good news? Most lower back pain is self-limiting. Research shows it often resolves within two weeks to a month with minimal intervention — especially in people under 60.
But when pain lingers, flares repeatedly, or starts affecting your work and daily life, you need a clear plan — not guesswork.
This guide walks you through every stage: from understanding what’s causing your pain, to proven treatments, to long-term prevention.
I’m Vasilios Nenos, founder of MAST Health and a licensed chiropractic physician with advanced training in clinical neurology, and I’ve built my practice around finding the root cause of lower back pain treatment challenges rather than just masking symptoms. My background includes hospital-based clinical research and years of hands-on rehabilitation work with patients across a wide range of spinal and neurological conditions.
Understanding the Root Causes of Lumbar Discomfort
To find the right lower back pain treatment, we first have to understand the “why” behind the “ouch.” Your lumbar spine is a marvel of engineering, but because it supports the entire weight of your upper body, it is remarkably prone to wear and tear.
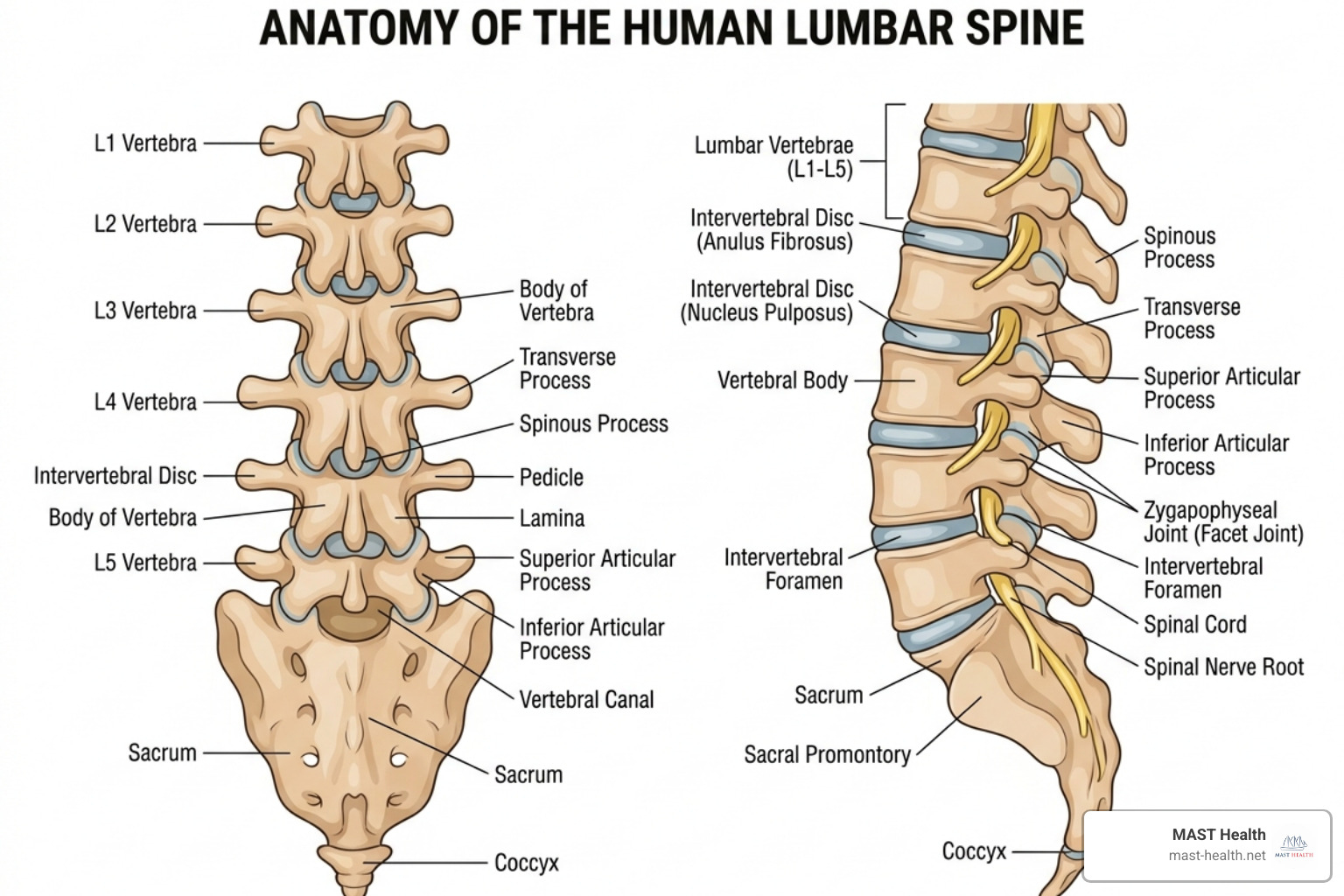
Most cases of lower back pain fall into a few specific categories:
- Muscle Strains and Ligament Sprains: These are the most common culprits. Whether you lifted a heavy box incorrectly or moved suddenly during a workout, microscopic tears in the soft tissues can lead to intense spasms and localized pain.
- Herniated or Bulging Discs: Your spinal discs act as shock absorbers. As we age (especially after age 30), these discs can lose moisture and flatten. If the soft inner material leaks out or the disc bulges, it can press against nearby nerves, causing radiating pain known as sciatica.
- Degenerative Disc Disease: This isn’t actually a “disease” but a natural part of aging where discs wear down. According to NIAMS, this can lead to morning stiffness and pain that worsens with sitting or bending.
- Spinal Stenosis: This is a narrowing of the spaces within your spine, which can put pressure on the nerves that travel through the spine. It’s often seen in adults over age 50.
- Spondylolisthesis: This occurs when one vertebra slips forward over the one below it. It’s particularly common in young athletes who perform repetitive hyperextension of the spine.
Beyond structural issues, lifestyle factors play a massive role. Obesity (a BMI over 25) significantly increases the mechanical force on your spine. Furthermore, smoking is a hidden enemy of back health; research indicates smokers are four times more likely to suffer from degenerative disc disease because nicotine restricts blood flow to the spinal discs.
Evidence-Based Lower Back Pain Treatment Strategies
When you’re in the thick of a pain episode, you want relief now. However, the most effective lower back pain treatment is often a “multipronged approach” rather than a single magic pill.
The Mayo Clinic and other leading medical institutions suggest starting with conservative, non-surgical options. Here is how to navigate the initial phase:
- Activity Modification: Gone are the days when doctors prescribed weeks of bed rest. We now know that bed rest can actually lead to muscle wasting and stiffness. Instead, we recommend “active rest”—continuing light activities like walking while avoiding heavy lifting or twisting.
- Pharmacologic Support: Over-the-counter (OTC) options like NSAIDs (ibuprofen or naproxen) or acetaminophen can help manage inflammation and pain. For chronic cases, some doctors may prescribe antidepressants like duloxetine, which have been shown to interrupt pain signals in the brain.
- Topical Treatments: Creams containing capsaicin or menthol can temporarily desensitize pain receptors, providing a window of relief so you can move more comfortably.
Temperature Therapy: Heat vs. Cold
One of the most frequent questions we hear at our Tampa FL clinic is whether to reach for the ice pack or the heating pad.
| Therapy | Best Used For | How it Works |
|---|---|---|
| Cold (Ice) | Acute injury (first 48-72 hours) | Reduces swelling and numbs sharp pain. |
| Heat | Chronic stiffness / tight muscles | Increases blood flow and relaxes tissues. |
Pro tip: Never apply ice or heat directly to the skin. Wrap it in a thin towel and limit sessions to 20 minutes to prevent skin damage.
Home Care and Self-Management
You are the most important member of your own recovery team. Effective lower back pain treatment continues at home through specific exercises and lifestyle tweaks:
- The Cat-Cow Stretch: On all fours, alternate between arching your back like a cat and sinking your belly toward the floor (the cow). This promotes mobility in the lumbar region.
- Knee-to-Chest: Lying on your back, gently pull one knee toward your chest and hold for 30 seconds. This helps decompress the lower spine.
- Ergonomic Adjustments: If you work at a desk in Tampa Bay, ensure your screen is at eye level and your feet are flat on the floor. Use a small rolled-up towel behind your lower back for lumbar support.
- Anti-Inflammatory Nutrition: Your diet impacts your pain levels. Incorporating turmeric (a natural anti-inflammatory), Vitamin D, and Magnesium can support muscle function and bone health.
Professional Nonsurgical Lower Back Pain Treatment
If home remedies aren’t cutting it, it’s time to seek professional intervention. At MAST Health, we emphasize a whole-body, root-cause approach.
- Physiotherapy and Corrective Exercise: Working with a professional for Physiotherapy Corrective Exercise ensures you are strengthening the right muscles—specifically your core and pelvic floor—to stabilize the spine.
- Chiropractic Adjustments: These Chiropractic Adjustments are designed to realign the spine, release compressed nerves, and restore joint mobility. It’s a natural, minimally invasive way to address mechanical issues.
- Acupuncture and Massage: These therapies can be excellent adjuncts to traditional care, helping to reduce muscle tension and stimulate the body’s natural pain-relieving chemicals.
- Cognitive Behavioral Therapy (CBT): For chronic sufferers, CBT helps manage the psychological toll of persistent pain, which is essential for long-term recovery.
According to the AAFP, first-line treatment should always prioritize these non-pharmacologic and non-surgical options before moving to more invasive measures.
When to Move Beyond Conservative Care
While 90% of back pain improves within six weeks, some situations require a more intensive lower back pain treatment plan.
The “Red Flags”
You should seek immediate medical attention if your back pain is accompanied by:
- Sudden loss of bowel or bladder control (a sign of Cauda Equina Syndrome).
- “Saddle anesthesia” (numbness in the groin or inner thighs).
- Progressive weakness in the legs that makes walking difficult.
- Unexplained weight loss or fever.
- Pain that is the result of a serious trauma, like a car accident.
Advanced Interventions
If conservative care fails after 6-12 weeks, your doctor might suggest:
- Imaging: While X-rays and MRIs aren’t usually needed for acute pain, they become necessary if symptoms persist or neurological deficits appear.
- Epidural Steroid Injections: These can provide temporary relief (usually 1-3 months) by reducing inflammation around a specific nerve root. As noted in AAFP guidelines, these are most effective when used as a “bridge” to allow you to participate in physical therapy.
- Radiofrequency Ablation: This procedure uses radio waves to damage specific nerves, blocking them from sending pain signals to the brain.
- Surgery: This is considered a last resort. It is typically only recommended for structural issues like severe disc herniation or spinal stenosis that haven’t responded to other treatments.
Long-Term Prevention and Lifestyle Integration
The best lower back pain treatment is the one you never have to repeat. Prevention is about building a “biological corset” of strong muscles to protect your spine.
- Core Strengthening: Focus on Pilates or yoga movements that engage the transverse abdominis (your deep core).
- Proper Lifting: Always bend at the knees, not the waist. Keep the object close to your body.
- Weight Management: Losing even five to ten pounds can significantly reduce the mechanical load on your lumbar discs.
- Movement Breaks: If you have a sedentary job in Tampa, set a timer for every 30 minutes to stand up, stretch, and walk for two minutes.
Our Physiotherapy Corrective Exercise programs are specifically designed to teach you these movement patterns so they become second nature.
The Role of Chiropractic in Lower Back Pain Treatment
Chiropractic care is often the “missing link” for many patients. At MAST Health, we specialize in Auto Accident Injury Rehabilitation. If you’ve been in a collision, the forces involved can dislodge vertebrae and tear soft tissue, leading to chronic issues if not addressed early.
Many people ask, “Should I See a Chiropractor After a Car Accident?” The answer is almost always yes. Early intervention can prevent the formation of scar tissue and ensure your spine heals in proper alignment. Whether you are an athlete seeking help from a Chiropractor in Tampa for Sports Injuries or a desk worker with “tech neck” and lower back strain, personalized wellness plans are the key to staying pain-free.
Frequently Asked Questions about Back Relief
How long does it take for lower back pain to go away?
Most acute lower back pain (lasting less than 4 weeks) improves significantly within two weeks. Subacute pain lasts up to 12 weeks. If pain persists beyond three months, it is classified as chronic. Fortunately, with the right lower back pain treatment, even chronic cases can see significant improvement.
When is surgery actually necessary for back issues?
Surgery is usually only considered when there is clear evidence of nerve compression (like a herniated disc) that is causing progressive muscle weakness or bowel/bladder issues, and only after 6-12 weeks of conservative treatment has failed. Surgery corrects structural problems but does not always guarantee the elimination of pain.
Can lifestyle changes really reverse chronic back pain?
Yes! While we can’t “reverse” arthritis or degenerative disc disease, we can absolutely change how your body handles the load. By strengthening supporting muscles, improving flexibility, and reducing systemic inflammation through diet and smoking cessation, many people with chronic conditions live virtually pain-free lives.
Conclusion
Lower back pain can feel like an insurmountable obstacle, but it doesn’t have to be your “new normal.” From the initial relief of an ice pack to the long-term stability provided by Chiropractic Adjustments, there is a clear path forward.
At MAST Health, we serve the Tampa Bay community with a focus on finding the root cause of your discomfort. We understand that your life doesn’t stop for back pain, which is why we offer weekend and same-day appointments at our Tampa FL location.
Ready to take the first step toward a stronger, more mobile you? Learn What to Expect on Your First Visit to Mast Health Chiropractic and explore Our Services today. Your spine—and your sanity—will thank you.
Recent Posts


Tampa Accident Physio for Fast Recovery




